Have you noticed your feet changing colour lately? Perhaps your toes have turned an alarming shade of purple, or you’ve spotted dark patches that weren’t there before?
Foot discolouration acts as your body’s early warning system – and these colour changes shouldn’t be dismissed as purely cosmetic concerns. When your feet turn purple, blue, white, or grey, you’re looking at potential circulation problems that could signal serious underlying health issues. These colour changes might indicate anything from Raynaud’s disease and peripheral arterial disease to frostbite.
The statistics tell a concerning story. Purple feet in elderly patients demand immediate attention, with stasis dermatitis affecting approximately 6-7% of patients older than 50 years. That dark spot on your foot or the consistently purple appearance? These changes often point to blood circulation problems requiring prompt medical evaluation. Most people first notice these symptoms during temperature extremes or after sitting or standing for extended periods.
But here’s the challenge: How do you know when these colour changes signal something serious versus a temporary issue?
This guide breaks down the different types of foot discolouration, reveals what they indicate about your health, and explains exactly when you need professional medical attention. You’ll discover the diagnostic methods doctors use, the conditions behind these symptoms, and proven treatment approaches that address the root causes.
Types of Foot Discolouration and What They Indicate
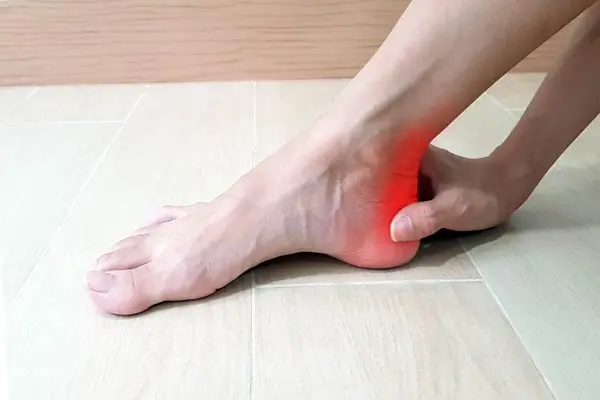
Your feet sit furthest from your heart, making them the canaries in the coal mine for circulation problems. Different colours tell different stories about what’s happening inside your blood vessels.
Blue or purple feet
Peripheral cyanosis – that’s the medical term when your feet turn blue or purple because they’re not getting enough oxygen-rich blood. Think of it like a traffic jam in your circulatory system.
Raynaud’s phenomenon ranks among the most common culprits. Your blood vessels in the extremities narrow excessively, causing toes to cycle through blue, white, purple, or red colours. The colour changes come with numbness, tingling, and sometimes pain or difficulty moving your toes.
Peripheral Arterial Disease (PAD) creates similar bluish or dark purple feet through narrowed or blocked arteries. The restricted blood flow triggers pain during walking – or even at rest in severe cases. Diabetes compounds this problem by damaging the tiny blood vessels in your feet, leading to both discolouration and wounds that heal poorly.
Brown or dark patches
Those rust-coloured or brownish patches appearing near your ankles have a name: hemosiderin staining. Blood leaks from tiny vessels called capillaries, leaving hemoglobin residue in the tissue. These stains often darken over time, sometimes appearing almost black.
This discolouration usually points to chronic venous insufficiency – your leg veins struggle to push blood back to your heart. The condition affects up to 40% of Americans, particularly those over 50 or anyone who’s had leg blood clots previously.
Redness and inflammation
Red feet span a spectrum from minor irritations to serious vascular conditions. Erythromelalgia causes burning pain alongside hot, red skin, primarily affecting the feet. Environmental allergens – grass, pollen, or cosmetic ingredients – can trigger redness with itching, swelling, and rashes.
Bacterial or fungal infections enter through breaks in your skin, producing redness, pain, discharge, and swelling. Athlete’s foot specifically targets the skin between toes and on the soles, creating redness, burning, and peeling.
White or pale areas
Blanching occurs when blood flow gets temporarily blocked, turning your skin white or paler than normal. You can test this yourself – gently press your skin and watch it turn lighter before returning to its normal colour.
Cold or stress can trigger Raynaud’s phenomenon in your toes, causing them to turn white initially before shifting to blue and finally returning to normal as blood flow improves.
How Doctors Diagnose the Cause
Getting to the root of foot discolouration requires medical expertise and a systematic diagnostic approach. Once you’ve noticed concerning changes in your feet’ appearance, a professional evaluation becomes essential for proper treatment planning.
Physical examination and visible signs
Your doctor’s assessment begins the moment you walk through the door. They observe your gait, note any walking aids you’re using, and examine your footwear for unusual wear patterns that might indicate abnormal foot contact with the ground.
The physical examination covers several key areas:
Visual inspection – Your doctor examines your feet for visible bruising, swelling, warmth, and areas of tenderness that provide clues about your condition.
Pulse assessment – Checking the strength of pulses in your feet is crucial, as significantly weaker or undetectable pulses often signal diminished blood flow – a key indicator of Peripheral Arterial Disease (PAD).
Skin and nail evaluation – Poor wound healing frequently suggests insufficient circulation to deliver nutrients for proper tissue repair, making this assessment particularly important.
Ultrasound and blood flow tests
Following the physical examination, doctors use various ultrasound techniques to visualise blood movement through your vessels. Colour duplex ultrasound creates detailed images of your veins using specialised software, helping identify blood clots, vessel changes, and reduced blood flow.
Doppler ultrasound shows the direction and speed of blood moving through arteries and veins. This non-invasive test produces coloured images revealing blood flow patterns without requiring injectable contrast dyes or radiation.
For a more detailed assessment, Magnetic Resonance Venography (MRV) combines magnetic fields and radio frequencies to generate detailed images of blood vessels throughout the affected areas.
Blood tests and oxygen levels
Blood analysis provides essential supporting evidence for diagnosing foot discolouration. While blood work alone cannot conclusively identify specific conditions, it reveals valuable information about contributing factors.
Standard tests often include:
- Cholesterol level evaluation
- Diabetes screening and monitoring
- Pulse oximetry to measure blood oxygen levels (particularly relevant for bluish discolouration)
- Arterial blood gas measurements for precise oxygen saturation data
When a skin biopsy is needed
Doctors recommend skin biopsies primarily when investigating persistent rashes, suspicious moles, or abnormal skin lesions that could indicate serious conditions. This procedure involves removing a small skin sample for laboratory analysis.
The process is straightforward: Most commonly, a punch biopsy technique is used, where the surrounding skin is numbed before taking the tissue sample. The biopsy site requires daily dressing changes until healing occurs – usually within 10-14 days.
Results typically return within one week, allowing your medical team to plan appropriate treatment based on definitive findings.
Underlying Conditions Behind Discolouration
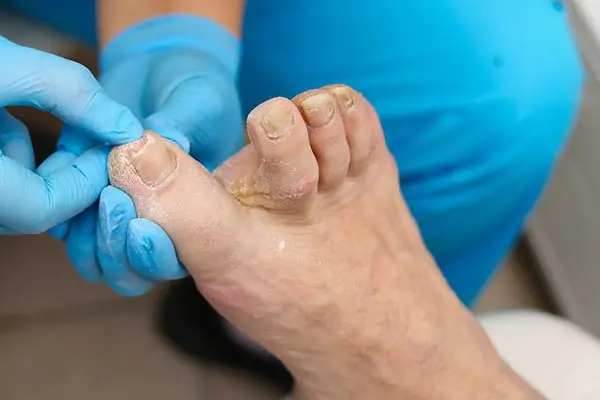
What’s actually causing those colour changes in your feet? The answer often lies in how specific medical conditions disrupt your body’s circulation and blood vessel function.
Vascular diseases like PAD and varicose veins
Peripheral Artery Disease (PAD) develops when fatty deposits accumulate in your arterial walls, creating bottlenecks that restrict blood flow to your feet. Think of it like a garden hose with kinks – the reduced oxygen delivery turns your feet blue or purple as they struggle to receive an adequate blood supply.
Varicose veins tell a different story. Here, damaged valves allow blood to flow backward instead of returning efficiently to your heart. Blood pools in your lower extremities, creating those swollen, purplish veins you can see beneath the skin surface.
Autoimmune and connective tissue disorders
Your immune system can become your feet’s worst enemy when autoimmune conditions develop. The statistics are sobering: approximately 9 in 10 people with scleroderma experience foot discolouration as their body’s defence system mistakenly attacks healthy connective tissue.
Lupus affects about 1 in 3 sufferers with circulation-related foot changes, while conditions like rheumatoid arthritis and Sjögren’s syndrome create similar problems through blood vessel inflammation. These conditions essentially turn your immune system against your own circulation network.
Diabetes and nerve damage
Diabetes creates a perfect storm for foot discolouration. High blood sugar levels gradually damage small blood vessels over time, reducing circulation and producing purple or blue discolouration. The real danger? Diabetic neuropathy often means you won’t feel wounds or infections developing, making early detection nearly impossible without regular foot inspections.
Cold-induced conditions like Raynaud’s and acrocyanosis
Cold weather can trigger dramatic colour changes in susceptible individuals. Raynaud’s phenomenon causes blood vessel spasms in your toes during cold exposure or emotional stress – affected areas turn white, then blue, before returning to red as blood flow normalises.
Acrocyanosis presents a more persistent problem, causing ongoing bluish discolouration from chronically narrowed small blood vessels. Unlike Raynaud’s, this condition affects hands and feet continuously, not just during cold triggers.
Important consideration: Many of these conditions overlap or occur together, which is why professional diagnosis becomes essential for proper treatment planning.
Treatment and Prevention Strategies
The key to managing foot discolouration lies in addressing the root cause rather than just treating surface symptoms. Early intervention makes all the difference – it can prevent complications and significantly improve your quality of life.
Compression therapy and circulation support
Compression therapy stands as the frontline defence against circulation-related foot discolouration. Medical compression stockings work by applying graduated pressure to your legs, essentially squeezing blood past faulty valves and back toward your heart instead of allowing it to pool in your lower extremities.
These therapeutic garments come in different pressure ratings:
- Low pressure: Less than 20 mmHg (available over-the-counter)
- Moderate pressure: 20-30 mmHg (often recommended for mild cases)
- High pressure: Greater than 30 mmHg (requires prescription and professional fitting)
Note: Elastic bandages and Velcro wraps provide viable alternatives for people who find compression stockings difficult to manage.
Medications for vascular and autoimmune issues
Medical treatment varies significantly depending on your specific condition. For Peripheral Arterial Disease (PAD), doctors typically prescribe a combination approach: antiplatelet drugs like aspirin prevent blood clots, statins tackle cholesterol levels, and blood pressure medications ensure optimal circulation.
Raynaud’s phenomenon responds well to calcium channel blockers, which help keep your arteries open and maintain healthy blood flow. Additional options include topical treatments – nicotinic acid derivatives and minoxidil can provide targeted relief for circulation-related discolouration.
Foot care for people with diabetes
Daily foot inspection becomes non-negotiable when you’re managing diabetes. Check for any colour changes, cuts, or swelling – including those hard-to-see areas between your toes. Use a mirror if needed, or ask someone to help with the inspection.
Essential diabetic foot care rules:
- Wear properly fitting shoes and socks at all times
- Protect feet from temperature extremes
- Never walk barefoot, even indoors (nerve damage means you might not feel injuries)
- Moisturise regularly, but avoid areas between toes
If you’re experiencing foot discolouration or any concerning symptoms, reach out to Coastal Podiatry for professional podiatry services and expert advice.
Lifestyle changes to improve blood flow
Simple daily habits can significantly impact your circulation. Elevate your legs above heart level for 30 minutes each day – this reduces swelling and encourages proper blood flow back to your heart.
Regular walking serves as one of the most effective treatments for poor circulation. Even moderate activity helps pump blood through your extremities more efficiently. Your diet matters too: foods rich in vitamins C and E support skin healing, while reducing sodium intake minimises swelling.
Important: Avoid staying in one position for extended periods – whether sitting or standing, movement keeps your circulation active.
When surgery or intervention is needed
Severe vascular conditions sometimes require more than conservative treatment. Modern medicine offers several minimally invasive options that deliver excellent results with faster recovery times.
Common procedures include:
- Endovenous ablation: Uses radiofrequency or laser energy to close abnormal veins
- Ultrasound-guided foam sclerotherapy: Injects a specialised solution into affected veins to seal them closed
- Ambulatory phlebectomy: Removes damaged surface veins through tiny skin punctures
For significant arterial blockages, bypass procedures might become necessary to restore proper blood flow to your feet.
Conclusion
Foot discolouration acts as your body’s early warning system – and now you understand exactly what these colour changes mean for your health.
The key takeaway? Early recognition saves complications. Whether you’re dealing with blue toes from Raynaud’s phenomenon, brown patches indicating venous insufficiency, or persistent redness suggesting infection, prompt professional evaluation makes all the difference.
Your diagnostic journey starts with a thorough physical examination, progresses through specialised testing such as ultrasound and blood analysis, and culminates in targeted treatment plans. Treatment options range from compression therapy and medications to lifestyle modifications – all tailored to address your specific underlying condition.
Special consideration for high-risk patients: If you’re living with diabetes or an autoimmune disorder, daily foot inspection isn’t optional—it’s essential. These conditions dramatically increase your risk of serious complications, making consistent foot care your first line of defence.
Here’s what you need to remember: Most foot discolouration responds exceptionally well to proper treatment when addressed quickly. Don’t dismiss those colour changes as purely cosmetic concerns or wait for symptoms to worsen.
If you’re experiencing foot discolouration or any symptoms discussed in this guide, contact Coastal Podiatry for professional podiatry services and expert evaluation. What appears minor today could develop into serious complications tomorrow – but with the right professional guidance, you can protect your foot health and maintain your quality of life.
Key Takeaways
Understanding foot discolouration can help you identify serious health conditions early and prevent complications through timely medical intervention.
- Blue or purple feet signal poor circulation – Often indicates conditions like Raynaud’s disease, PAD, or diabetes requiring immediate medical evaluation.
- Brown patches suggest chronic venous problems – Hemosiderin staining from blood vessel leakage affects up to 40% of Americans over 50.
- Early diagnosis prevents serious complications – Doctors use physical exams, ultrasound, and blood tests to identify underlying vascular or autoimmune conditions.
- Daily foot inspection is crucial for diabetics – Check for colour changes, wounds, and swelling to prevent dangerous complications from nerve damage.
- Treatment ranges from compression therapy to surgery – Options include medical stockings, medications, lifestyle changes, and minimally invasive procedures, depending on severity.
Don’t ignore persistent foot discolouration – what seems like a cosmetic issue could be your body’s early warning system for serious circulatory or health problems that respond best to prompt medical attention.




